
The Province needs to pay physicians more
by: Perry Lupyrypa and Sam Rogers
Dr. Ramsay Hijazi, speaking on behalf of the Ontario Union of Family Physicians (OUFP) says there are about 5,500 family doctors in Ontario trained to do family medicine. Rather than running a family practice they are choosing to work in other areas, like cosmetic medicine or in a hospital.
The OMA reports the Ministry of Health is currently paying family physicians 37 percent of previous rates
Hijazi says the Ontario Medical Association (OMA) keeps track of whether OHIP rates have kept up with inflation and rising expenses over time. The OMA reports the Ministry of Health is currently paying family physicians 37 percent of previous rates. He says many family physicians are losing money so many are leaving their practices. And it’s affecting medical students too.
“When we talk about the shortage of family doctors, we actually don’t have a shortage. We actually have an excess of family doctors. What we have a shortage of is family doctors who are trained to do family medicine, who are actually practicing family medicine”
— Dr Ramsay Hijazi, Ontario Union of Family Physicians (OUFP)
The Canadian Resident Matching Service (CaRMS) reports there are more than enough medical student and resident student positions across Canada. Data shows an increasing trend of unfilled training spots since 2021 with the first quarter of 2024 peaking at 108 unfilled training spots out of a total of 558. Major cities like London and Kingston have unfilled training spots.
Dr Sohail Gandhi, family physician in Stayner, Ontario says with the way things are he can’t in good conscience tell the younger medical students of today to go into practicing family medicine. He says things need to change and they need to change drastically.
In an open letter to all family practice residents by Gandhi and family physicians Drs. Nadia Alam and Silvy Mathew wrote it is “unsafe to run a family practice in Ontario, especially for those just starting.”
By 2026, the OMA is projecting one in four Ontarians will be without a family doctor. Dr. Mekalai Kumanan, president of the Ontario College of Family Physicians (OCFP) says approximately 70 percent of Ontarians without a family doctor also don’t have access to team-based care.
Ian Warford, 34, from Etobicoke has been without a family physician since moving to Toronto in 2016. He says having a family doctor and regular check ups would improve his quality of life. Suffering from chronic knee pain since 2009, after a truck hit and dragged him while out for a walk, Warford says he resorts to visiting random doctors at walk-in clinics when in need.
Hijazi says since 2016, front line physicians have been warning about burnout in family medicine. In 2021 OMA reports 73 percent of physicians experience some level of burnout. In 2017 when a survey showed nearly 70% of 1000 Ontario family physicians responding they were facing burnout. That rate was double the national average of 35 percent. In 2021 OMA reports 73 percent of physicians experience some level of burnout.
“The digital health branch of the ministry of health and e-health Ontario have underperformed.”
— Dr. Sohail Ghandi
Gandhi says some of the pain is because “ digital health IT in Ontario is a complete disaster.” Using covid vaccinations as an example, Gandhi says he can’t get the covid vaccine entered into the electronic database – even though there is an on-line system. When a patient gets a Covid-19 vaccine at a pharmacy, the pharmacist updates the online system. Duplicating efforts, the family physician then manually enters that vaccination into the Ontario health system. Complicating matters is when a patient gets a SARS-CoV-2 test at a hospital. Family physicians are informed about the test. But not given any results. The doctor must download the procedure to get results.
Gandhi says he pushed for a unified solution when he was president of the OMA. It didn’t go through.
Physicians are business people too
The OMA reports the vast majority of physicians are not government employees but independent contractors and small-business owners providing patients a service then billing OHIP. As such, these small business owners are not eligible for employer benefits, pensions, paid vacation, or sick leave. Using fees received through billing all overhead must be paid – including staff salaries and benefits, office space, medical equipment and supplies, electronic health records, utilities and more. The OMA reports an average physician’s overhead is about 30 percent of gross billings and can be higher. The OMA also reports family physicians spend on average, 19 hours a week on unpaid paperwork.
France Gelinas is the NDP Health Critic and MPP for Nickel Belt. She says Ontario’s healthcare system has never been in such a crisis with over 1,200 Hospital service closures, over 200 emergency room closures and 2.3 million Ontarian’s without access to Primary Care because they don’t have a family doctor .
In March 2024, Ontario’s Leader of the Opposition Marit Stiles put forth a resolution to free up doctors’ time by getting them access to an integrated primary care team. Styles said this would be equivalent to adding 2,000 doctors to the system. The motion did not pass, with Progressive Conservative MPPs voting down the idea.
The Ontario government says a heath team connects patients to a range of health professionals working together under one roof. This includes doctors, nurse practitioners, registered and practical nurses, physiotherapists, social workers and dietitians, among others. They say they want to ensure families access timely, quality primary care and improve access to care for patients without a family doctor, especially in rural, remote, and underserved areas.
Hijazi says his clinic is a team-based care model and his clinic loses money every single year, He says the only way clinics stay open is if physicians lose money and use personal income to keep the clinic open, He says with inflation of the last few years everything has come to a head and that’s why there’s physicians are now talking about it.
Exploring solutions – What the Ontario government is doing
Over the past 15 months Sylvia Jones, Deputy Premier and Minister of has Health has made two announcements, one each giving pharmacists and nurses additional responsibility; three announcements supporting primary health care teams bringing total spending of $546 million over the next three years; and as part of the April budget announcing building Canada’s first medical school at York University for students studying to be primary care physicians. Below is a timeline of Ontario Ministry of Health announcements since January 2023.
Timeline Cycle Visual Charts by plupyrypa
Ramsay says building more medical schools will not solve the family physician shortage. Ghandi agrees.
“While Ontario building medical schools is great future planning, absolutely something has to be done in the here and now, right now to stabilize the hemorrhage of are people leaving comprehensive family practice.”
— Dr. Sohail Ghandi
Exploring solutions – Some nurse practitioners (NP) are opening up private clinics
The website for IHolistic Solutions, a new private medical clinic in Ancaster says they provide affordable private nurse practitioner led family health care for anyone looking for comprehensive family health care or looking for same day appointments. Their website says because NPs are not covered by OHIP, they can bill patients privately.
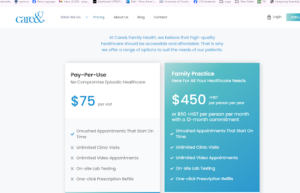
Other private nurse practitioner led (NPL) clinics are opening up across the province. At care& in Toronto patients can sign up for $450 per person per year, or pay $75 per visit.
Gelinas says in her riding of Capreol a nurse opened a private NPL clinic because she wasn’t able to serve all the patients in the public clinic. Gelinas says “The nurse practitioner who opened the clinic said, and I will quote her words, “Had the Capreol clinic received funding to hire a permanent position, I would have likely stayed there.”
Are Family Practice Doctors needed?
A recent study from Norway reported hospital admissions reduced by about 30 percent and mortality rates lower by about 25 percent for patients having a regular general practitioner for more than 15 years compared to having one for one year.
Exploring solutions -The Ontario College of Family Physicians (OCFP) proposal
Since 2022, the OCFP has been warning of a growing crisis because they are expecting a wave of early retirements, are experiencing COVID-related backlogs and soaring demands for care, and increasing needs from population growth and aging. They want to solve the problem and are proposing three policy recommendations:
- Ensure Ontarians have a family doctor working alongside a team, so patients can get the help they need faster.
- Improve the accessibility of care by increasing the time that family doctors can spend providing direct patient care.
- Ensure every Ontarian has a family doctor by recruiting and retaining more family doctors within the province.
Hijazi says the net income of Ontario family physicians has fallen 21% since 2021.
Gandhi says the simple solution is “ pay the family physicians more, like Manitoba and B.C. have. This must be done now to stabilize the hemorrhaging of family physicians leaving.”




Be the first to comment